Question from health professional: “How do you feel?”
Answer from me: “Sad… not happy”.
Pain is multidimensional. The experience of pain is not generated from physiological processes alone. Considering the multidimensionality of pain is especially important for both 1) understanding why chronic pain has such a large impact on peoples’ lives, and 2) for developing effective pain management for each person.
There are many models of pain that try to capture the varied dimensions of pain. In biopsychosocial models (1), there are sensory, affective, cognitive, and behavioural dimensions1. There are many variants of biopsychosocial models so I’ll outline the general way these dimensions are described.
The sensory dimension is the “pain” part of the pain experience. This includes physiological processes and systems, such as activation of nociceptors (free nerve endings in our periphery which are sensitive to heat and cold, pressure, or chemicals).
The cognitive aspect is the thoughts or “cognitions” about pain that a person has. For example, not being able to stop thinking about pain.
The behavioural dimension is the action or inactions associated with pain. For example, avoiding certain movements.
The affective dimension is the emotional feelings a person with chronic pain may have about their pain. For example, feeling scared that the pain might never go away.
These dimensions do not occur in a vacuum. A person lives in a social environment: family, friends, work, communities, countries. These social environments affect the immediate sensory, cognitive, behavioural and affective dimensions too.
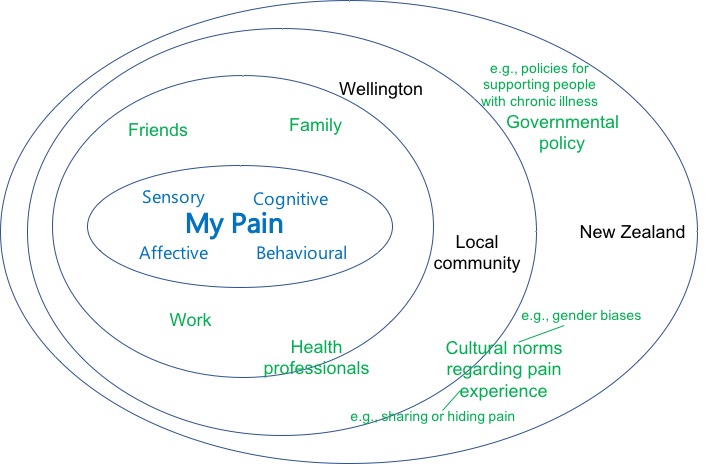
To explore the importance of considering chronic pain in a biopsychosocial context start with the articles the Biopsychosocial Model Helps Explain Complex Differences in Pain and The Experience of Chronic Pain: Many Dimensions, Lots of Uniqueness.
I’m going to give a personal example to illustrate the importance of considering the affective dimension in pain management.
In 2012 I was assessed by a group of health professionals at a Pain Management Clinic. I was in the midst of the worst flare up of my fibromyalgia that I had experienced (and is still the worst I have had). When I went to the Pain Management Clinic, I did not know a lot about pain or pain management.
One of the concerns identified in this assessment was that I could not name my emotions. When asked how I felt, I could only reply “sad” and “not happy”, which to any person seeing me would have seemed like a huge understatement.
At this point in time, my pain was out of control, I was taking large amounts of codeine, taking other medicines to manage the side effects of taking so much codeine, and the one way I knew how to cope – pushing my pain aside until later – had stopped working. I was deeply depressed. I had resigned from my job and was basically spending most of my day in bed. And all I could say, was “sad” and “not happy”.
When I was then asked just to name emotions, I couldn’t even write a list. This was quite shocking to me. My honours and masters research in psychology had been on emotional language. I had spent hours thinking, reading, and writing about emotions. Yet, I could not list emotions. There are quite a lot of emotional feelings or states!
Happy, sad, angry, fearful, surprise, disgust are basic emotions, and then there are all their nuances; delighted, distraught, steaming, terrified, shocked, revolted to name a few. And all I could say, was “sad” and “not happy”.
Alexythimia describes this inability to name emotions you are experiencing or that are being experienced by others.
At the end of this first visit to the Pain Management Clinic, I had learned that it wasn’t just the sensory dimension of pain that was stopping me from managing my pain and living my life. All dimensions of my pain needed to be addressed.
It is easier to change some dimensions than others. Thoughts and behaviours are the easiest (though by no means easy!). In the next pinch, I’m going to give a personal example to illustrate the importance of considering the cognitive dimension in pain management.
[1] Some biopsychosocial models have three dimensions.
- Asmundsen, G. J. G. & Wright, K. D. (2012). Biopsychosocial approaches to pain. In T. Hadjistavropoulos & K. D. Craig (Eds.), Pain: Psychological Approaches (pp. 35–57). New York: Psychology Press.

Pingback: Thoughts (3) – the b word – Pinches of Pain blog